Effect of warm ischemia time of donor liver from donation after cardiac death on transplant liver in rats
-
摘要:
目的 评价大鼠心脏死亡器官捐献(DCD)供肝热缺血时间对移植肝的影响。 方法 建立大鼠DCD供肝原位肝移植模型。根据供肝获取前经历心脏停搏时间的不同, 将54只受体大鼠分为3组:对照组(W0组, 未经历热缺血)、热缺血10 min组(W10组)、热缺血20 min组(W20组), 每组18只。各组大鼠分别于术后1、3、7 d检测血清肝功能[丙氨酸转氨酶(ALT)和天冬氨酸转氨酶(AST)], 电子显微镜观察肝细胞及其细胞器, 用蛋白质免疫印迹(Western blot)法检测肝组织细胞色素C(Cyt C)和凋亡诱导因子(AIF)的蛋白表达水平。 结果 随着热缺血时间的延长, 肝移植术后1 d, 各组大鼠ALT和AST水平急剧上升, 与W0组相比, W10组和W20组的ALT和AST水平均明显升高(均为P < 0.05)。术后3 d, 各组大鼠ALT和AST水平均稍稍下降, 与W0组相比, W10组和W20组的ALT和AST水平仍明显较高(均为P < 0.05)。术后7 d, 各组大鼠ALT和AST水平均再次上升, 与W0组相比, W10组和W20组的ALT和AST水平升高更显著(均为P < 0.05)。电子显微镜观察发现, 随着热缺血时间的延长, 肝细胞水肿程度逐渐加重, 内质网扩张逐渐加重, 线粒体损伤程度加重, W20组尤为严重。术后1 d, 3组大鼠肝组织中的AIF和Cyt C蛋白表达水平的比较, 差异均无统计学意义(均为P > 0.05)。术后3、7 d, 与W0组比较, W10组和W20组的AIF与Cyt C蛋白表达水平均较高, 差异均有统计学意义(均为P < 0.05), 且W20组的AIF与Cyt C蛋白表达水平均高于W10组(均为P < 0.05)。 结论 DCD供肝热缺血主要损伤肝细胞, 随着热缺血时间的延长, 移植肝肝细胞内线粒体和其他细胞器形态、及线粒体凋亡相关蛋白水平均出现明显变化。 Abstract:Objective To evaluate the effect of warm ischemia time of donor liver from donation after cardiac death (DCD) on transplant liver in rats. Methods The rat models of orthotopic liver transplantation of DCD donor liver were established.According to the time of cardiac arrest before obtaining the donor livers, 54 recipient rats were evenly divided into three groups:control group (W0 group, no warm ischemia, n=18), 10 min warm ischemia group (W10 group, n=18) and 20 min warm ischemia group (W20 group, n=18).At 1, 3, and 7 d after operation, serum liver function [alanine aminotransferase (ALT) and aspartate aminotransferase (AST)] were quantitatively measured in rats of each group, liver cells and its organelles were observed by electron microscopy and the expression levels of cytochrome C (Cyt C) and apoptosis inducing factor (AIF) proteins in liver tissues were detected by Western blot in rats of each group. Results The serum levels of ALT and AST in each group were significantly increased at 1 d after liver transplantation along with the prolongation of warm ischemia time.Compared with the W0 group, the serum levels of ALT and AST in the W10 and W20 groups were increased significantly (all P < 0.05).At postoperative 3 d, the serum levels of ALT and AST in each group were slightly decreased.Compared with the W0 group, the serum levels of ALT and AST in the W10 and W20 groups were significantly higher (all P < 0.05).At 7 d after operation, the serum levels of ALT and AST in each group were elevated again.Compared with the W0 group, the serum levels of ALT and AST in the W10 and W20 groups were remarkably increased (all P < 0.05).Electron microscope showed that along with the prolongation of warm ischemia time, the degree of hepatocyte edema was gradually aggravated, the endoplasmic reticular expansion was steadily increased and the degree of mitochondrial damage was aggravated, especially in the W20 group.At postoperative 1 d, the expression level of AIF and Cyt C proteins in the liver tissues did not significantly differ among three groups (all P > 0.05).At 3 and 7 d after operation, compared with the W0 group, the expression levels of AIF and Cyt C proteins were significantly up-regulated in the W10 and W20 groups (all P < 0.05), and the expression levels of AIF and Cyt C proteins in the W20 group were significantly higher than those in the W10 group (both P < 0.05). Conclusions The warm ischemia of the DCD donor liver mainly leads to liver cell injury.Along with the extension of warm ischemia time, significant changes occur in the morphology of mitochondria and other organelles and the expression level of mitochondrial apoptosis-related proteins in transplanted liver cells. -
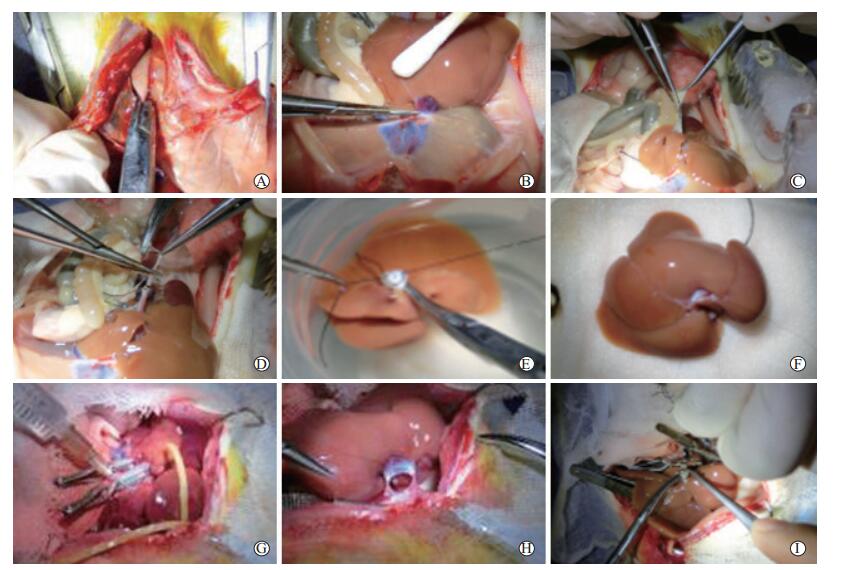
图 2 各组大鼠肝移植术后不同时间点肝组织超微结构变化(×10 000)
A图示W0组术后1 d, 可见粗面内质网扩张, 线粒体未见肿胀, 嵴排列整齐, 未见断离及溶解; B图示W0组术后3 d, 可见肝细胞水肿, 部分粗面内质网扩张, 线粒体未见明显异常; C图示W0组术后7 d, 可见肝细胞水肿, 部分内质网扩张, 线粒体未见明显异常; D图示W10组术后1 d, 可见肝细胞水肿明显, 内质网及线粒体未见明显异常; E图示W10组术后3 d, 可见肝细胞水肿, 胆汁残体, 其余未见明显异常; F图示W10组术后7 d, 可见肝细胞水肿, 部分线粒体固缩, 脂质残体, 其余未见异常; G图示W20组术后1 d, 可见肝细胞水肿, 肝血窦充血, 线粒体嵴排列整齐, 部分嵴溶解, 可见胆汁残体; H图示W20组术后3 d, 可见肝细胞水肿, 部分粗面内质网扩张, 其余未见异常; I图示W20组术后7 d, 可见肝细胞水肿明显, 细胞出现坏死, 部分线粒体水肿、固缩、崩解及坏死
Figure 2. Ultrastructural changes of liver tissue at different time points after liver transplantation in rats of each group
表 1 各组大鼠肝移植术后不同时间点肝功能水平的比较
Table 1. Comparison of liver function at different time points after liver transplantation in rats of each group(x±s, U/L)
组别 n 术后1 d 术后3 d 术后7 d ALT AST ALT AST ALT AST W0组 6 101.0±60.8 409.7±10.40 094.5±0.7 218.0±4.20 246.5±0.7 755.0±2.80 W10组 6 260.2±27.5 686.5±106.3 101.5±0.7 250.0±18.4 305.0±1.4 995.0±14.1 W20组 6 246.0±1.40 458.5±3.500 147.5±0.7 284.3±1.40 732.0±4.2 2 527.0±17.00 F值 0.184 0.361 0.256 0.441 1.000 1.000 P值 0.000 0.000 0.000 0.000 0.000 0.000 -
[1] 丁利民, 徐志丹, 李新长, 等.公民逝世后器官捐献供肝保护及功能评估临床分析[J].器官移植, 2017, 8(6):430-434.DOI: 10.3969/j.issn.1674-7445.2017.06.004.DING LM, XU ZD, LI XC, et al.Clinical analysis on donor liver protection and function evaluation for organ donation after citizen's death[J].Organ Transplant, 2017, 8(6):430-434.DOI: 10.3969/j.issn.1674-7445.2017.06.004. [2] ISHIKAWA T, SHIMADA S, FUKAI M, et al.Post-reperfusion hydrogen gas treatment ameliorates ischemia reperfusion injury in rat livers from donors after cardiac death:a preliminary study[J].Surg Today, 2018, DOI:10.1007/s00595-018-1693-0[Epubahead of print]. [3] 邓永林, 沈中阳.我国心脏死亡器官捐献的现状及影响因素[J].中华外科杂志, 2012, 50(8):673-674.DOI: 10.3760/cma.j.issn.0529-5815.2012.08.001.DENG YL, SHEN ZY.The present situation and influencing factors of donation after cardiac death in China[J].Chin J Surg, 2012, 50(8):673-674.DOI: 10.3760/cma.j.issn.0529-5815.2012.08.001. [4] 董权, 李超, 王胤佳, 等.中国实行心脏死亡器官捐献供体的可行性分析[J].中国普外基础与临床杂志, 2012, 19(5):498-501. http://d.old.wanfangdata.com.cn/Periodical/zgpwjcylczz201205010DONG Q, LI C, WANG YJ, et al.Feasibility analysis of organ donation after cardiac death in China[J].Chin J Bases Clin Gen Surg, 2012, 19(5):498-501. http://d.old.wanfangdata.com.cn/Periodical/zgpwjcylczz201205010 [5] 尹志科, 严谨.心脏死亡器官捐献的困境及对策[J].医学与哲学, 2012, 33(1):28-29, 32. http://d.old.wanfangdata.com.cn/Periodical/yxyzx201201009YIN ZK, YAN J.The predicament of organ donation after cardiac death and its countermeasures[J].Med Philos, 2012, 33(1):28-29, 32. http://d.old.wanfangdata.com.cn/Periodical/yxyzx201201009 [6] 杨春华, 陈雪霞, 谢文锋, 等.器官捐献与供体维护[J].新医学, 2013, 44(6):363-365.DOI: 10.3969/g.issn.0253-9802.2013.06.002.YANG CH, CHEN XX, XIE WF, et al.Organ donation and donor maintenance[J].New Med, 2013, 44(6):363-365.DOI: 10.3969/g.issn.0253-9802.2013.06.002. [7] COFFEY JC, WANIS KN, MONBALIU D, et al.The influence of functional warm ischemia time on DCD liver transplant recipients'outcomes[J].Clin Transplant, 2017, 31(10).DOI: 10.1111/ctr.13068. [8] 刘学民, 王博, 于良, 等.心脏死亡供体经典原位肝移植的单中心临床研究[J].器官移植, 2013, 4(1):23-27.DOI: 10.3969/j.issn.1674-7445.2013.01.005.LIU XM, WANG B, YU L, et al.Single-center clinical study of orthotopic liver transplantation using donation after cardiac death[J].Organ Transplant, 2013, 4(1):23-27.DOI: 10.3969/j.issn.1674-7445.2013.01.005. [9] NEVES DB, RUSI MB, DIAZ LG, et al.Primary graft dysfunction of the liver:definitions, diagnostic criteria and risk factors[J].Einstein(San Paulo), 2016, 14(4):567-572.DOI: 10.1590/S1679-45082016RW3585. [10] KAMADA N, CALNE RY.A surgical experience with five hundred thirty liver transplants in the rat[J].Surgery, 1983, 93(1 Pt 1):64-69. https://www.ncbi.nlm.nih.gov/pubmed/6336859 [11] 中华医学会器官移植学分会.中国肝移植乙型肝炎防治指南(2016版)[J].临床肝胆病杂志, 2017, 33(2):213-220.DOI: 10.3969/j.issn.1001-5256.2017.02.002.Branch of Organ Transplantation of Chinese Medical Association.The practice guideline on prophylaxis and treatment of hepatitis B for liver transplantation in China (2016 edition)[J].J Clin Hepatol, 2017, 33(2):213-220.DOI: 10.3969/j.issn.1001-5256.2017.02.002. [12] POMPILI M, FRANCICA G, PONZIANI FR, et al.Bridging and downstaging treatments for hepatocellular carcinoma in patients on the waiting list for liver transplantation[J].World J Gastroenterol, 2013, 19(43):7515-7530.DOI: 10.3748/wjg.v19.i43.7515. [13] 沈中阳.供肝短缺背景下我国肝癌患者肝移植的策略[J].中华器官移植杂志, 2013, 34(9):513-515.DOI: 10.3760/cma.j.issn.0254-1785.2013.09.001.SHEN ZY.Strategy of liver transplantation for liver cancer patients in China under the background of liver donor shortage[J].Chin J Organ Transplant, 2013, 34(9):513-515.DOI:10.3760/cma.j.issn.0254-1785.2013. 09.001. [14] 黄洁夫.创建符合中国国情的器官捐献与移植体系[J].中华外科杂志, 2013, 51(1):1-3.DOI: 10.3760/cma.j.issn.0529-5815.2013.01.001.HUANG JF.Establishment of organ donation and transplantation system in accordance with China's national conditions[J].Chin J Surg, 2013, 51(1):1-3.DOI: 10.3760/cma.j.issn.0529-5815.2013.01.001. [15] 侯萍, 李剑平.器官移植前保存的理论研究与临床应用[J].中国组织工程研究, 2012, 16(5):895-898.DOI: 10.3969/j.issn.1673-8225.2012.05.031.HOU P, LI JP.Clinical application and theoretical study of organ preservation before transplantation[J].Chin J Tissue Eng Res, 2012, 16(5):895-898.DOI: 10.3969/j.issn.1673-8225.2012.05.031. [16] 张静, 李胜兰, 吴媛, 等.定位在线粒体的肝刺激因子对线粒体膜电势的影响[J].中国组织化学与细胞化学杂志, 2013, 22(2):89-94.DOI: 10.3870/zgzzhx.2013.02.001.ZHANG J, LI SL, WU Y, et al.Effect of HSS on mitochondrial membrane potential[J].Chin J Histochem Cytochem, 2013, 22(2):89-94.DOI: 10.3870/zgzzhx.2013.02.001. [17] 宋冬梅, 陈丽, 马俊香, 等.锰对SH-SY5Y细胞线粒体超微结构及功能改变的研究[J].实用医学杂志, 2017, 33(5):680-683.DOI:10.3969/j.issn.1006-5725. 2017.05.002.SONG DM, CHEN L, MA JX, et al.Mitochondrial ultrastructure and function changes in SH-SY5Y induced by manganese[J].J Pract Med, 2017, 33(5):680-683.DOI: 10.3969/j.issn.1006-5725.2017.05.002. [18] KAKIZAKI Y, MIYAGI S, SHIMIZU K, et al.The effects of short-term subnormothermic perfusion after cold preservation on liver grafts from donors after circulatory death:an ex vivo rat model[J].Transplantation, 2018, 102(4):e147-e154.DOI: 10.1097/TP.0000000000002080. [19] LIU Z, PAN N, LV X, et al.Orthotopic liver transplantation from cardiac death donors in the mouse:a new model and evaluation of cardiac death time[J].Iran J Basic Med Sci, 2017, 20(6):683-689.DOI: 10.22038/IJBMS.2017.8838. -





 下载:
下载: